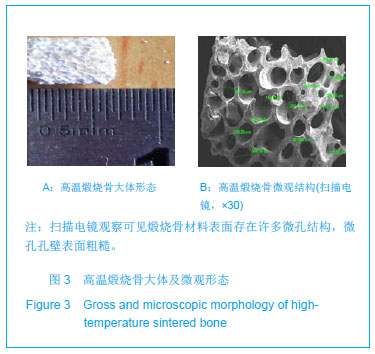
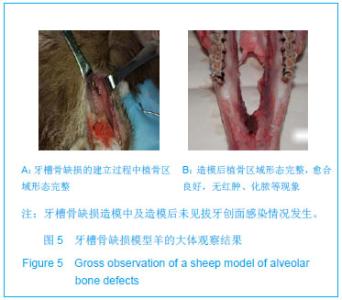
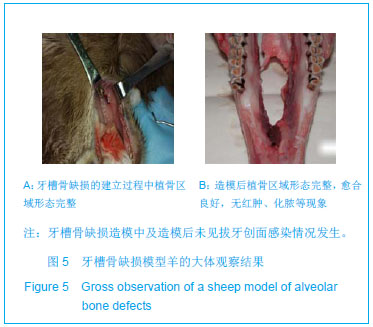
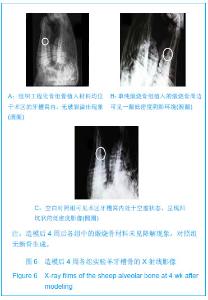
Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (34): 6089-6096.doi: 10.3969/j.issn.2095-4344.2013.34.005
Previous Articles Next Articles
Tissue-engineered bone repairs sheep alveolar bone defects
Zhang Qin, Yang Chuan-bo, He Hui-yu, Cui Jie, Yang Nan, Ma Wen-yuan
- Department of Prosthodontics, First Affiliated Hospital of Xinjiang Medical University, Urumqi 830054, Xinjiang Uygur Autonomous Region, China
-
Online:2013-08-20Published:2013-08-20 -
Contact:He Hui-yu, M.D., Professor, Master’s supervisor, Chief physician, First Affiliated Hospital of Xinjiang Medical University, Urumqi 830054, Xinjiang Uygur Autonomous Region, China hehuiyu02@sina.com -
About author:Zhang Qin, Master, Attending physician, Department of Prosthodontics, First Affiliated Hospital of Xinjiang Medical University, Urumqi 830054, Xinjiang Uygur Autonomous Region, China zhangqin678ok@163.com -
Supported by:the National Natural Science Foundation of China, No. 81060088*;
the Natural Science Foundation of the Science and Technology Bureau of Xinjiang Uygur Autonomous Rgion, No. 2011211A073*;
the Youth Fund of Affiliated Hospital of Xinjiang Medical University, No. 2012QN21*
CLC Number:
Cite this article
Zhang Qin, Yang Chuan-bo, He Hui-yu, Cui Jie, Yang Nan, Ma Wen-yuan. Tissue-engineered bone repairs sheep alveolar bone defects[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(34): 6089-6096.
share this article
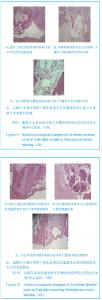
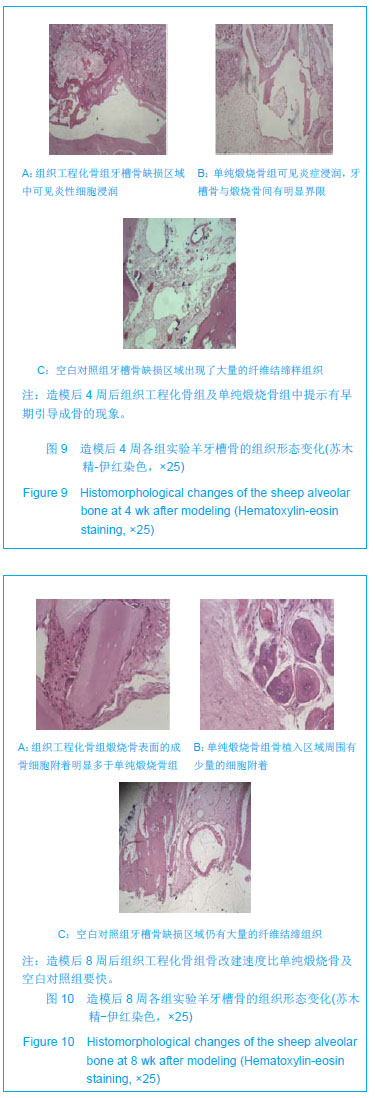
2.7 组织工程化骨修复羊牙槽骨的组织病理结果 造模后4周:单纯煅烧骨组和组织工程化骨组牙槽骨缺损区域中均可见炎性细胞浸润。在牙槽骨缺损区域周围和煅烧骨材料之间有明显的界限,视野中可发现局部有未降解的煅烧骨材料残片,可能是在制作病理切片时所致,提示新生骨组织的改建仍在进行过程中。在空白对照组牙槽骨缺损区域出现了大量的纤维结缔样组织,分布较为广泛,呈不规则状,见图9。 造模后8周:单纯煅烧骨组和组织工程化骨组中的骨植入区域周围有少量的细胞附着,经进一步观察证实为骨母细胞,为早期的骨组织细胞,提示新生牙槽骨组织正处于改建过程中。通过对比发现组织工程化骨组煅烧骨表面的成骨细胞附着明显多于单纯煅烧骨组,说明了组织工程化骨组的骨改建及诱导新生骨过程早于单纯煅烧骨组。空白对照组中观察可见牙槽骨缺损区域仍有大量的纤维结缔组织充斥,与周围的骨组织呈不连续状态,见图10。"
| [1]张淅,姚遥,刘迎飞.牙周炎致骨缺损的植骨治疗[J].临床口腔医学杂志,2010,26(5):292-294.[2]Somerman MJ, Ouyang HJ, Berry JE, et al. Evolution of periodontal regeneration: from the roots' point of view. J Periodontal Res. 1999;34(7):420-424.[3]Kubota K, Yoshimura N, Yokota M, et al. Overview of effects of electrical stimulation on osteogenesis and alveolar bone. J Periodontol. 1995;66(1):2-6.[4]童庆春,李宁毅,张志勇,等.即刻骨移植与延期牙种植术联合应用修复牙槽骨缺损的初步研究[J].上海口腔医学,2008,17(5): 488-491.[5]朱淑倩,何家才.人工骨替代材料修复种植体周围骨缺损的研究进展[J].医学综述,2010,16(6):863-865.[6]游永刚,唐辉,徐永清.不同骨移植材料骨诱导活性的研究现状[J].现代生物医学进展,2008,8(7):1338-1339.[7]杨川博,何惠宇.牙槽骨缺损修复治疗新进展[J].中国实用口腔科杂志,2012,3(5):182-185.[8]刘世森,苏方,刘洪臣.组织工程骨修复种植部位骨量不足的临床进展[J]中华老年口腔医学杂志,2009,7(3):180-182.[9]Griffith LG, Naughton G. Tissue engineering--current challenges and expanding opportunities. Science. 2002; 295(5557):1009-1014.[10]王敏,翁雨来,胡晓洁,等.组织工程技术修复犬牙槽骨缺损的实验研究[J].中华医学杂志,2003,83(15):1339-1344.[11]许慧芬,何惠宇,唐小雪,等.不同方法制备异种骨支架材料的生物相容性评价[J].中国组织工程研究与临床康复,2011,15(47): 8749-8752.[12]Weng Y, Cao Y, Silva CA, et al. Tissue-engineered composites of bone and cartilage for mandible condylar reconstruction. J Oral Maxillofac Surg. 2001;59(2):185-190.[13]Shang Q, Wang Z, Liu W, et al. Tissue-engineered bone repair of sheep cranial defects with autologous bone marrow stromal cells. J Craniofac Surg. 2001;12(6):586-595.[14]杨川博,何惠宇,崔杰,等.骨髓基质干细胞复合煅烧骨的皮下成骨[J].中国组织工程研究,2013:17(16):2883-2890.[15]中华人民共和国科学技术部. 关于善待实验动物的指导性意见. 2006-09-30.[16]唐小雪,何惠宇,许慧芬等.两种不同分离方法对羊骨髓间充质干细胞生物活性的影响[J].中国组织工程研究与临床康复,2011, 15(49):9137-9140.[17]Erdemli O, Captug O, Bilgili H, et al. In vitro and in vivo evaluation of the effects of demineralized bone matrix or calcium sulfate addition to polycaprolactone-bioglass composites. J Mater Sci Mater Med. 2010;21(1):295-308. [18]Jähn K, Braunstein V, Furlong PI, et al. A rapid method for the generation of uniform acellular bone explants: a technical note. J Orthop Surg Res. 2010;5:32. [19]Lin FH, Liao CJ, Chen KS, et al. Preparation of a biphasic porous bioceramic by heating bovine cancellous bone with Na4P2O7.10H2O addition. Biomaterials. 1999;20(5):475-484.[20]崔杰.去抗原异种松质骨支架材料的制备及性能研究[D].乌鲁木齐:新疆医科大学.2011.[21]许慧芬,何惠宇,唐小雪,崔杰.物理联合化学或化学方法处理去抗原异种松质骨支架与骨髓间充质干细胞的细胞相容性[J].中国组织工程研究,2012,02(5):958-962.[22]唐小雪,何惠宇,许慧芬,等.两种不同分离方法对羊骨髓间充质干细胞生物活性的影响[J].中国组织工程研究与临床康复,2011, 15(49):9137-9140.[23]王文良,张华亮,初殿伟,等.自体骨髓间充质干细胞复合壳聚糖/羟基磷灰石支架修复兔膝骨软骨缺损[J].中华骨科杂志,2009, 29(1):61-64.[24]孟焕新.牙周病学[M].北京:人民卫生出版社,2008.[25]孙路,王永兰.牙周组织工程研究新进展[J].牙体牙髓牙周病学杂志,2012,3:170-174. [26]宋珂,曹颖光.多元化骨组织工程修复颌骨缺损的研究进展[J].临床口腔医学杂志,2010,26(2):125-127.[27]陈广东,杨惠林,王根林,等.骨髓间充质干细胞的成骨分化及临床应用[J].中国组织工程研究与临床康复,2010,14(49): 9272-9276.[28]Caplan AI. Mesenchymal stem cells. J Orthop Res. 1991;9(5): 641-650.[29]Derubeis AR, Cancedda R. Bone marrow stromal cells (BMSCs) in bone engineering: limitations and recent advances. Ann Biomed Eng. 2004;32(1):160-165.[30]Hasegawa N, Kawaguchi H, Hirachi A, et al. Behavior of transplanted bone marrow-derived mesenchymal stem cells in periodontal defects. J Periodontol. 2006;77(6):1003-1007.[31]Caplan AI, Dennis JE. Mesenchymal stem cells as trophic mediators. J Cell Biochem. 2006;98(5):1076-1084.[32]Maniatopoulos C, Sodek J, Melcher AH. Bone formation in vitro by stromal cells obtained from bone marrow of young adult rats. Cell Tissue Res. 1988;254(2):317-330.[33]Weng Y, Wang M, Liu W, et al. Repair of experimental alveolar bone defects by tissue-engineered bone. Tissue Eng. 2006; 12(6):1503-1513.[34]Hayashi O, Katsube Y, Hirose M, et al. Comparison of osteogenic ability of rat mesenchymal stem cells from bone marrow, periosteum, and adipose tissue. Calcif Tissue Int. 2008;82(3):238-247. [35]Prockop DJ. Marrow stromal cells as stem cells for nonhematopoietic tissues. Science. 1997;276(5309):71-74.[36]柴岗,张艳,刘伟,等.人骨髓基质细胞表面标志的研究[J].组织工程与重建外科杂志,2005,1(5):263-264.[37]Minamide A, Tamaki T, Kawakami M, et al. Experimental spinal fusion using sintered bovine bone coated with type I collagen and recombinant human bone morphogenetic protein-2. Spine (Phila Pa 1976). 1999;24(18):1863-1872.[38]Barnes B, Boden SD, Louis-Ugbo J, et al. Lower dose of rhBMP-2 achieves spine fusion when combined with an osteoconductive bulking agent in non-human primates. Spine (Phila Pa 1976). 2005;30(10):1127-1133.[39]Tamaki T, Sakurai K, Kasamatsu N. Results of basic and clinical studies of true bone ceramic. In: Urist MR, O'Connor BT, Burw ell RG, eds. Bone Grafts, Derivatives and Substitute. Oxford: Buterworth Heinemann,1994.[40]Katoh T, Sato K, Kawamura M, et al. Osteogenesis in sintered bone combined with bovine bone morphogenetic protein. Clin Orthop Relat Res. 1993;(287):266-275.[41]Lin FH, Liao CJ, Chen KS, et al. Preparation of betaTCP/HAP biphasic ceramics with natural bone structure by heating bovine cancellous bone with the addition of (NH(4))(2)HPO(4). J Biomed Mater Res. 2000;51(2):157-163.[42]Le Huec JC, Schaeverbeke T, Clement D, et al. Influence of porosity on the mechanical resistance of hydroxyapatite ceramics under compressive stress. Biomaterials. 1995;16(2): 113-118.[43]Lane JM, Bostrom MP. Bone grafting and new composite biosynthetic graft materials. Instr Course Lect. 1998;47: 525-534.[44]许永华,施新猷,胡蕴玉,等.牛煅烧骨与体外培养兔骨膜成骨细胞的相容性[J].第四军医大学学报,2000,21(4):512-514.[45]Sandberg MM, Aro HT, Vuorio EI. Gene expression during bone repair. Clin Orthop Relat Res. 1993;(289):292-312.[46]Wilson CE, Dhert WJ, Van Blitterswijk CA, et al. Evaluating 3D bone tissue engineered constructs with different seeding densities using the alamarBlue assay and the effect on in vivo bone formation. J Mater Sci Mater Med. 2002;13(12):1265- 1269.[47]Kruyt M, De Bruijn J, Rouwkema J, et al. Analysis of the dynamics of bone formation, effect of cell seeding density, and potential of allogeneic cells in cell-based bone tissue engineering in goats. Tissue Eng Part A. 2008;14(6):1081- 1088. [48]van Gaalen SM, de Bruijn JD, Wilson CE, et al. Relating cell proliferation to in vivo bone formation in porous Ca/P scaffolds. J Biomed Mater Res A. 2010;92(1):303-310. |
| [1] | Hua Haotian, Zhao Wenyu, Zhang Lei, Bai Wenbo, Wang Xinwei. Meta-analysis of clinical efficacy and safety of antibiotic artificial bone in the treatment of chronic osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 970-976. |
| [2] | Zhang Bin, Sun Lihua, Zhang Junhua, Liu Yusan, Cui Caiyun. A modified flap immediate implant is beneficial to soft tissue reconstruction in maxillary aesthetic area [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 707-712. |
| [3] | Li Chenjie, Lü Linwei, Song Yang, Liu Jingna, Zhang Chunqiu. Measurement and statistical analysis of trabecular morphological parameters of titanium alloy peri-prosthesis under preload [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 516-520. |
| [4] | Li Li, Ma Li. Immobilization of lactase on magnetic chitosan microspheres and its effect on enzymatic properties [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 576-581. |
| [5] | Liu Liu, Zhou Qingzhu, Gong Zhuo, Liu Boyan, Yang Bin, Zhao Xian. Characteristics and manufacturing techniques of collagen/inorganic materials for constructing tissue-engineered bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 607-613. |
| [6] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [7] | He Jie, Chang Qi. Biological reconstruction of large bone defects after resection of malignant tumor of extremities [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 420-425. |
| [8] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [9] | Chen Siqi, Xian Debin, Xu Rongsheng, Qin Zhongjie, Zhang Lei, Xia Delin. Effects of bone marrow mesenchymal stem cells and human umbilical vein endothelial cells combined with hydroxyapatite-tricalcium phosphate scaffolds on early angiogenesis in skull defect repair in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3458-3465. |
| [10] | Zhou Anqi, Tang Yufei, Wu Bingfeng, Xiang Lin. Designing of periosteum tissue engineering: combination of generality and individuality [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3551-3557. |
| [11] | Zhang Zhenhua, Liu Zichen, Yu Baoqing. Status and problems of polycaprolactone and its composite materials in bone tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3571-3577. |
| [12] | Lang Limin, He Sheng, Jiang Zengyu, Hu Yiyi, Zhang Zhixing, Liang Minqian. Application progress of conductive composite materials in the field of tissue engineering treatment of myocardial infarction [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3584-3590. |
| [13] | He Fan, Xiong Xiuli, Shan Xianfeng, Zhang Shutong, Hu Jian, Wang Xuejin. Guided bone regeneration in a small animal model of critical size craniofacial bone defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3226-3231. |
| [14] | Xie Jian, Su Jiansheng. Advantages and characteristics of electrospun aligned nanofibers as scaffolds for tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(16): 2575-2581. |
| [15] | Ji Qi, Yu Zhengwen, Zhang Jian. Problems and trends of technique and clinical application of metallic biomaterials prepared by three-dimensional printing technology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(16): 2597-2604. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||